This calculator was last updated on 23/08/2021. It is currently not being updated regularly.
So far, COVID-19 has cost the world hundreds of billions of dollars and caused over 2 million casualties - over 5399 of these have been in Wales. We all think that COVID-19 has been our guest for way too long - but what can we do about it? The most effective way to battle this kind of enemy is to create a vaccine against it 💉. Multiple companies have been in a race since COVID-19 was discovered to do just that.
On 8 December 2020, the first person in Wales received a COVID-19 vaccine approved for general use. This event truly marks the beginning of the end of our COVID-19 troubles. But this raises a whole load of new questions:
- How far are we away from the finish line?
- Who will be first in the queue to get the vaccine?
- When are you likely to be offered it?
We created this calculator to deliver all the answers to every single one of these crucial questions. Omni's vaccine queue calculator will estimate for you how many people are ahead of you in the queue to get a COVID vaccine in Wales. It also predicts how long you might have to wait to get your vaccine. By using our tool, you'll have a better idea of when you can expect to get vaccinated.
We've based our vaccine queue calculator on the (which the Welsh government is also following) and the likely average rate of vaccination.
Time and time again, we've learnt that prevention is better than cure. A few steps toward hygiene can help you reduce the risk of COVID-19 infection. Our coronavirus mask calculator and isolation impact calculator will show you the effectiveness of small but important measures like wearing masks in public and social distancing.
Prioritising who gets the vaccine
It's great that we now have COVID vaccines that have been approved for general use. However, that's not the end of the COVID story just yet. Millions of doses of vaccines now have to be produced and injected into the arms of people. That is one massive manufacturing, logistical, and time-consuming task for everyone involved. A quick use of our vaccine production calculator will tell you that it is all going to take time.
The first phase of the vaccination programme focuses on saving lives and reducing hospital admissions. So it is logical to give the vaccine first to those groups that are most vulnerable - older people and those with pre-existing conditions.
The UK government has published a of groups that will get a COVID vaccine in the first phase. All four nations of the UK are following this priority list. Let's take a look at the list.
Priority list
Phase 1
- Residents in a care home for older adults and their carers;
- All those 80 years of age and over and frontline health and social care workers;
- All those 75 years of age and over;
- All those 70 years of age and over and clinically extremely vulnerable individuals;
- All those 65 years of age and over;
- All individuals aged 16 years to 64 years with underlying health conditions which put them at higher risk of serious disease and mortality. Unpaid carers who receive carer's allowance or are the main carer of an elderly or disabled person;
- All those 60 years of age and over;
- All those 55 years of age and over; and
- All those 50 years of age and over.
Phase 2
For Phase 2, priority will be based on age, to make the rollout as simple and as quick as possible:
- All those aged 40 to 49 years;
- All those aged 30 to 39 years; and
- All those aged 18 to 29 years.
We have gathered data on how big each group is likely to be (see graphic below), so we can estimate where you are in the queue.
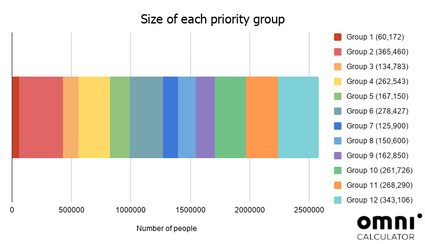
So you know whether you are included in a particular group, let's examine them in detail.
Clinically extremely vulnerable individuals
If you received a letter from your GP asking you to shield yourself during lockdown, then you are included in this group.
If you are not sure, here is a list of conditions that automatically qualify you in this group:
-
Solid organ transplant recipients;
-
People with specific cancers:
- People with cancer who are undergoing active chemotherapy;
- People with lung cancer who are undergoing radical radiotherapy;
- People with cancers of the blood or bone marrow such as leukaemia, lymphoma or myeloma who are at any stage of treatment;
- People having immunotherapy or other continuing antibody treatments for cancer;
- People having other targeted cancer treatments that can affect the immune system, such as protein kinase inhibitors or PARP inhibitors; and
- People who have had bone marrow or stem cell transplants in the last six months or who are still taking immunosuppression drugs.
-
People with severe respiratory conditions including all cystic fibrosis, severe asthma and severe chronic obstructive pulmonary disease (COPD);
-
People with rare diseases that significantly increase the risk of infections (such as severe combined immunodeficiency (SCID), homozygous sickle cell disease);
-
People on immunosuppression therapies sufficient to significantly increase risk of infection;
-
Conditions involving the spleen, e.g. splenectomy (having your spleen removed);
-
Adults with Down’s syndrome;
-
Adults on dialysis or with chronic kidney disease (stage 5);
-
Women who are pregnant with significant heart disease, congenital or acquired; or
-
Other people who have also been classed as clinically extremely vulnerable, based on clinical judgement and an assessment of their needs. GPs and hospital clinicians have been provided with guidance to support these decisions.
[Source: ]
Underlying health conditions
If you currently have one of the listed underlying health conditions, you are at increased risk from COVID-19:
- Chronic respiratory disease, including chronic obstructive pulmonary disease (COPD), cystic fibrosis, and severe asthma;
- Chronic heart disease (and vascular disease);
- Chronic kidney disease;
- Chronic liver disease;
- Chronic neurological disease or condition, including epilepsy;
- Chronic liver disease;
- Down’s syndrome;
- Severe and profound learning disability (everyone on the GP's learning disability register);
- Diabetes;
- Solid organ, bone marrow, and stem cell transplant recipients;
- People with specific cancers (e.g., leukaemia, lymphoma, myeloma, etc.);
- People who have suffered a stroke or a transient ischaemic attack (TIA);
- A neurological or muscle wasting condition;
- Immunosuppression due to disease (e.g., HIV) or treatment;
- Asplenia and splenic dysfunction (e.g., sickle cell disease, removed spleen, etc.);
- Morbid obesity (BMI of 40 and higher); or
- Severe mental illness.
Whether you are offered the vaccine may depend on the severity of your condition. Your GP can advise on
whether you are eligible.
[Source: ]
Pregnancy and breastfeeding
If you are currently pregnant or are planning a pregnancy in the next three months, then . This is an update to the previous advice and will help protect more people. The evidence for this change comes from over 90,000 pregnant women vaccinated in the US with mRNA vaccines (Pfizer and Moderna) with no safety concerns being raised.
On 30 December, now allows both the Pfizer-BioNTech and AstraZeneca vaccines to be offered to women while breastfeeding. This change of advice is because there is no known risk with giving non-live vaccines to breastfeeding women. However, there is an absence of safety data specifically for the current COVID vaccines, which should be made clear to you before you give consent to have the vaccine.
Children
At this time, COVID vaccines are not being offered to people under 16 years of age, except in cases where there is a very high risk of exposure and severe outcomes. A full risk and benefits assessment is needed before administering the vaccine.
Again, as more trial data become available, this recommendation may change.
❗ Disclaimer: Please remember that this calculator is based on the and does not take into consideration individual cases that might be exempt from this general prioritization.
How to use the vaccine queue calculator?
Follow these steps to calculate your likely place in the COVID vaccine queue. The first section is all about you.
- Please enter your age in years (16 to 120). Generally, the older you are, the sooner you'll be called up to have the vaccine.
- Say whether you live or work in a care home. If everyone in a care home is vaccinated, that will allow relatives to visit with decreased risk to the residents.
- Are you pregnant, or are you planning to be in the next three months? If the answer is yes, then you will be offered either the Pfizer or Moderna vaccine.
- Answer whether you are a frontline health or social care worker (e.g., nurse, doctor, etc.). This group is likely to have a lot of exposure to the virus and need to be protected.
- Are you classed as extremely vulnerable? Answer yes if you are asked to shield during lockdown or have one of the conditions on clinically extremely vulnerable individuals list in the previous section.
- Have you got one of the underlying health conditions mentioned in the previous section?
You will then see an estimate of the minimum and the maximum number of people who are inline to receive the vaccine before you. We also indicate how long it might be before you get both doses of the vaccine and be fully protected, based on the vaccination rate. By default, we base these figures on a plan by the Welsh government of to reach a milestone of 740,000 vaccines by mid-February. A default uptake rate is set to 69%. If you want to change these values, we'll explain how in the next section.
Rollout of vaccines section
In the Rollout of vaccines section of the calculator, you can change the figure of the vaccination rate used in the calculator. This is the rate at which people receive one dose of a vaccine. You can either choose:
- The Welsh government's planned rate. Currently, 150,000/week to reach a milestone of 740,000 vaccines by mid-February 2021.
- The last 7 days of vaccine doses administered. See help text for the current value.
- Or enter your own custom value.
You can also enter the time it will take to vaccinate everyone in Wales that wants the vaccine (takes into account the estimated uptake rate).
Not everyone who is asked to receive the vaccine will accept it. That will mean that the queue for you will, in effect, be shorter. We set a default uptake rate of 69%, which was for people aged 64 and over who accepted the annual flu vaccine. For COVID-19, the uptake may well be higher. Keep an eye out for the latest figure for the uptake rate and use it in the calculator.
We know that waiting to get the vaccine might be frustrating. However, by prioritising those people that are most at risk of hospitalisation and death, we should quickly be able to save lives with this fantastic new weapon against the virus.
Check out these other useful COVID-related tools:
Changelog
17 February 2021
-
If the real uptake rate of a group is higher than the overall uptake rate, then that group is considered complete.
-
Due to improvements in the calculations, if you are not in a priority group, you might see your dates slip.
4 March 2021
-
Added Phase 2 priority groups, 10-12.
-
Revised priority group population size estimates.
29 March 2021
- Calculations now considers the proportion of first doses to second doses administered in the last week. This will help account for the expected slowdown in rate of first dose being administered in April.
20 April 2021
- Updated the advice for pregnant women, who will now be offered either the Pfizer or Moderna vaccine.
15 May 2021
- Those in priority groups 9 and below will now get their second dose 8 weeks after their first dose (down from the usual 12 weeks). The calculator has been updated to reflect this change.
FAQs
Are COVID-19 vaccines safe?
COVID-19 vaccines that have been approved by the UK Medicines and Healthcare products Regulatory Agency (MHRA) will have passed all their safety tests. However, as with any approved drug on the market, you may experience side effects. Generally, though, the risk of side effects is much smaller than the possible consequences of a nasty COVID-19 infection.
How many shots of the COVID-19 vaccine will I need?
Nearly all COVID-19 vaccines approved or under development need two shots to be effective. The doses need to be around 3 to 12 weeks apart, depending on the vaccine. For example, you need to have the two Pfizer/BioNTech shots 21 days apart, while the Oxford/AstraZeneca vaccine can be up to 12 weeks apart. However, going forward, it is now the policy of the UK government to offer the second dose of both these vaccines 12 weeks after the first, to help more people get at least some protection sooner.
What are the possible side effects I might experience?
As with all vaccines, you might experience mild to moderate side effects that may last a few days. If you have pain and/or a fever, you can treat these side effects by taking medicines such as paracetamol. Below are the known side effects, grouped by frequency.
Very common (may affect more than 1 in 10 people):
- Pain at the injection site
- Tiredness
- Headache
- Muscle pain
- Chills
- Joint pain
- Fever
Common (may affect up to 1 in 10 people):
- Injection site swelling
- Redness at the injection site
- Nausea
Uncommon (may affect up to 1 in 100 people):
- Enlarged lymph nodes
- Feeling unwell
Will COVID vaccines be mandatory?
The UK government has said that COVID-19 vaccines will not be mandatory. However, you may have to get vaccinated to be allowed to do certain activities. An example is the Australian airline Qantas, which will require all passengers to be vaccinated once vaccines are widely available. So while you can technically opt-out of getting a COVID-19 vaccine, the practical restrictions on your life might be significant.
Who was the first person to receive a COVID-19 vaccine in Wales?
Care home worker Craig Atkins from Ebbw Vale was among the first people to receive the vaccine in Wales on 8 December 2020.
When was the first COVID-19 vaccine approved for the UK?
On the 2nd of December 2020, UK regulators approved the Pfizer/BioNTech vaccine on an emergency-use basis. This date was just seven months after clinical trials started. They were able to do this at super fast speed by analysing the trial data continuously, rather than waiting until the end of all the trials.
Who is making the COVID vaccine?
Two COVID-19 vaccines have been approved and are currently being administered and are made by Pfizer/BioNTech and AstraZeneca (in partnership with Oxford University). Many other vaccines are in development by companies such as GSK, Moderna, and Johnson & Johnson, to name but a few.
Will there be enough vaccine for everyone?
Certainly not at the moment, but eventually, yes. Pfizer alone plans to produce 1.3 billion doses of its vaccine in 2021. As further vaccines are approved and manufactured, more supply will come on stream to meet the demand around the world.
Do I still need to wear a mask after I am vaccinated?
Yes. At this stage, it is still unclear whether the current vaccine will also prevent the transmission of the virus to people around you. It is similar to the current situation where people have COVID-19 but suffer no symptoms. However, they are still able to transmit it to others. It may be only until a good majority of people have been vaccinated that restrictions to our daily lives are lifted.
What percentage needs to get vaccinated to achieve herd immunity?
We do not yet know the precise threshold of vaccinated people in the community needed to stop the spread of COVID-19 and achieve herd immunity. For flu, experts say the figure is around 70%, so that is the current working theory for COVID-19. Further research and modelling are needed to get a more concrete value.
If I've had COVID-19, do I need to be vaccinated?
Yes. If you have had COVID-19, then your body will have some natural immunity to it, preventing you from suffering from it again. However, some early evidence suggests this natural immunity might not last very long. While we also don't know precisely how long the vaccine's protection lasts, it could be better than your natural immunity. It will undoubtedly extend the time you are resistant to COVID-19.
Can I have a COVID-19 vaccine if I am currently breastfeeding?
Yes. The current advice now allows both the Pfizer-BioNTech and AstraZeneca vaccines to be offered to women while breastfeeding. That is because there is no known risk with giving non-live vaccines to breastfeeding women.
Do I get special priority if I am an unpaid carer?
Yes. Unpaid carers appear in group 6 on the UK government's nine-point priority list. If you receive carer's allowance or are the main carer of an elderly or disabled person who wouldn't receive their care if you fell ill, then you are included in this group.