This peak flow calculator allows you to calculate your normal peak expiratory flow (PEF), as well as your peak expiratory flow ratio (PEFR). The ratio is a relation between your measured PEF and the normal value, or, if you know it — your personal best. PEFR is a valuable, useful, and easy-to-obtain parameter in asthma control and management. You can also use a peak flow chart to find your normal peak flow value. At the end of the text, you can also read a short set of instructions on how to use a peak flow meter and obtain the proper result.
If you're interested in diseases of the respiratory system, check out our rapid shallow breathing index calculator.
We try our best to make our Omni Calculators as precise and reliable as possible. However, this tool can never replace a professional doctor's assessment. If any health condition bothers you, consult a physician.
What is peak expiratory flow ratio — PEFR?
Peak expiratory flow (PEF, or peak expiratory flow ratio — PEFR) is the maximum speed of air during expiration. The speed depends on three basic parameters: lung volume, strength of the respiratory muscles, and bronchial diameter. As the volume of the lungs remains almost the same for the entirety of adult life, and the respiratory muscles don't change their function day-to-day, any change in daily PEF measurements must reflect the level of bronchoconstriction.
PEFR is measured with a small, simple device called peak flow meter. See the section below to read how to use it correctly.
Why and when we measure peak expiratory flow?
As peak flow measures bronchial diameter, people at risk of rapid bronchoconstriction will benefit from it. These are mostly patients with asthma. While it can never replace spirometry, the standard lung examination, but regular peak flow measurements are recommended in some cases:
- Moderate and severe cases of asthma.
- Newly diagnosed cases of asthma.
- When a patient's asthma medicine has been adjusted.
- Occupational asthma.
Your peak flow should be checked in accordance with the plan you agree with your leading physician. Doctors can have few aims when it comes to peak flow measurements — sometimes, they want to check the diurnal variability and, sometimes, the response to new medications. A particular case is occupational asthma, where measurements should be done on workdays as well as during weekends and holidays — using a peak flow meter allows the physician to compare the measurements, and helps to state the right diagnosis. The lung function may also be estimated using spirometry — this similar test allows us to find, e.g., FEV1/FVC ratio and asses the level of bronchoconstriction.
🔎 If you find that interesting, you might want to check the vital capacity calculator and lung capacity calculator as well!
How to use a peak flow calculator?
Using the peak flow calculator is very simple. You only need to provide it with your data! Follow the steps below:
-
Fill in all the fields that describe you or your patient.
-
The result seen below is the estimated peak expiratory flow for the data you provided.
-
If you have performed an examination with a peak flow meter, you can input that reading into the calculator. If you do, it will calculate the zone that you're in. They are marked with colors, so it's easy to understand, even if you are a kid!
-
Also, if you have been using a peak flow meter for a while, you may be familiar with your personal best. You can note it down in the calculator and count the zones based on this reading. This is a better assessment option if you're monitoring your disease with PERF regularly. The thing is that estimation is always based on statistics and not your personal condition. This is why referring to your own values will give you a better perspective.
-
In the Diurnal variability section, you can input the greatest and smallest peak flow readings from one day. Diurnal variation is a valuable parameter for controlling asthma.
Peak flow chart
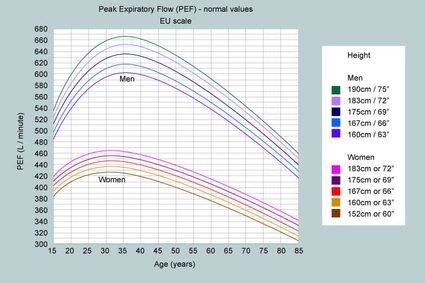
Besides using the peak flow calculator to get your value, there is also the option of reading it from a nomogram, in this case a peak flow chart. It doesn't take race into account, and it's age-limited (it won't show peak expiratory flow for children), but it is user-friendly, especially for people who like to see things in graphical form. Using a normal peak flow chart is popular, especially across Europe.
A peak flow chart can also refer to a kind of 'peak expiratory flow diary', that you can keep and record your PERF in. Some patients will find it better than just writing the daily results down.

How to use a peak flow meter?
A peak flow meter is a simple hand-held device. Most people are perfectly fine using it at home if their health provider gave them instructions before. As in peak expiratory flow, we need to measure the maximum speed of the air, so you cannot breath normally - it needs to be the fast blast kind of breath.

Reading the following instructions can help you:
-
Before attempting the breath, check if the marker (e.g., an arrow) is set in the lowest possible position — zero.
-
Stand up straight. You shouldn't be sitting, as it may interfere with the measurements.
-
Take a deep breath — as deep as you can!
-
Put the mouthpiece of the peak flow meter into your mouth and close your lips around it tightly. Take care of your tongue — it shouldn't block the airway.
-
Blow out as hard and as fast as you can.
-
The air coming from your lungs will force the marker to move along the scale and point to your result. Write it down.
-
Repeat steps 1-6 three times. If the tests were done correctly, the results should not differ from one another too much.
-
The highest result is the one you should consider as your result. You can now compare it to the average, standardized value, or your personal best in our peak flow calculator, to see in which zone you are in.
-
If needed, the peak flow calculator can also count the diurnal variability for you. Normal peak flow variability shouldn't exceed 20%.
If you measure your peak flow regularly, you should always do that at the same time of the day, as PEFR changes throughout the day.
Peak expiratory flow classification — color zones
A system based on the three traffic light colors is an easy and intuitive way to interpret the result of your PEFR measurement. However, there are two essential things to remember: Even if you are in the green zone but feel unwell (tightness in your chest, shortness of breath, or your inability to work and play like you usually do), you should consult your doctor. Also, PEFR diminishing over time may precede asthma exacerbation, even if you feel good.
The table below shows a summary of the color system:
Reading (% of estimation / personal best) | Color | Comment | What to do |
|---|---|---|---|
≥80% |  | Your disease is under control | Enjoy the day |
50-79% |  | Your airways are narrowing - your disease is poorly controlled | Take rescue medicine; if it doesn't bring relief, the symptoms are worsening, or you're back in the yellow zone in 4 hours - contact your doctor |
<50% |  | Your airways are severely narrowed | Use emergency medicine and contact professional health care immediately! |