The SAPS II calculator, or the Simplified Acute Physiology II Score calculator, is a tool that is used on patients admitted to Intensive Care Units who are aged 15 or older. It helps assess the severity of the disease and allows for ICU mortality rate calculations. Identifying patients with a high mortality risk is essential when you're planning an effective and efficient health care service, and so the SAPS II calculator is very useful.
We try our best to make our Omni Calculators as precise and reliable as possible. However, this tool can never replace a professional doctor's assessment. All information on this website is for informational purposes only and is not intended to serve as a substitute for medical consultation. Always consult your results with a health care provider.
How does the SAPS II calculator work?
The SAPS II test is a tool that is used exclusively on patients admitted to ICUs. What is ICU in medical terms? ICU stands for Intensive Care Unit (also: Intensive Therapy Unit), a special department of a hospital that treats severely ill patients who require constant care. The continuous care is provided by specialised physicians, nurses, and therapists. Patients may be referred to the ICU directly from the Emergency Room, after an invasive surgery, or when they deteriorate on a ward.
The score is calculated from 12 physiological measurements and three disease-related variables.
In each category a certain number of points is assigned to the patient - the worse the state or prognostics, the more points assigned. The result is an integer point score between 0 and 163, and the predicted mortality risk varies between 0% and 100%.
Definitions of categories used in SAPS II calculator
Below you can find descriptions of the terms used in this calculator. The points given to each answer are given in brackets:
-
Vitals
-
Age - for each age bracket, the patient receives a certain number of points: <40 years (0), 40-59 years (7), 60-69 years (12), 70-74 years (15), 75-79 years (16), ≥80 (18)
-
Heart rate - <40 bpm (11), 40-69 bpm (2), 70-119 bpm (0), 120-159 bpm (4), ≥160 bpm (7). If the patient had both cardiac arrest (11) and extreme tachycardia (7), assign the HR with the most points.
-
Systolic blood pressure - <70 mmHg (13), 70-99 mmHg (5), 100-199 mmHg (0), ≥200 mmHg (2). If it varies from 60 mmHg to 205 mmHg, assign 13 points.
-
Temperature - ≥39ºC or 102.2ºF (3), <39ºC or 102.2ºF (0)
-
Glasgow coma scale - 14-15 (0), 11-13 (5), 9-10 (7), 6-8 (13), <6 (26). If the patient is sedated, give an estimated Glasgow coma score from before sedation.
-
-
Oxygenation
- The patient is not on mechanical ventilation or CPAP (0)
- The patient is on mechanical ventilation or CPAP. The assigned value depends on the PF ratio calculator results: <100 mmHg/% or 13.3 kPa/% (11), 100-199 mmHg/% or 13.3-26.5 kPa/% (9), ≥200 mmHg/% or 26.6 kPa/% (6). Don't worry; the tool will calculate it for you. You only need the patient's PaO2 (partial pressure of oxygen measured from arterial blood) and FiO2 (fraction of inspired oxygen).
-
Renal
-
Urinary output - <500 ml/day (11), 500-999 ml/day (4), ≥1000 ml/day (0). If the patient is in the ICU for less than 24 hours, give the urine volume collected in 1 hour or calculate it for 24 hours.
-
Serum urea or BUN - put in the highest value in mmol/dL for serum urea or mg/dL for serum urea nitrogen (BUN): BUN <28 or urea <100 (0), BUN 28-83 or urea 10-29 (6), BUN ≥84 or urea ≥30 (10)
-
-
Chemistry
-
Serum sodium- use the worst value (the one with the most points assigned): <125 mEg/L (5), 125-144 mEq/L (0), ≥145 mEq/L (1)
-
Serum potassium - use the worst value (the one with the most points assigned): <3.0 mEq/L (3), 3.0-4.9 mEq/L (0), ≥5.0 mEq/L (3)
-
Bicarbonate - use the lowest value: <15 mEq/L (6), 15-19 mEq/L (3), ≥20 mEq/L (0)
-
Bilirubin - use the highest value: <4.0 mg/dL or <68.4 µmol/L (0), 4.0-5.9 mg/dL or 68.4-102.5 µmol/L (4), ≥6.0 mg/dL or ≥102.6 µmol/L (9)
-
-
Other
-
WBC count - input the worst white blood cells count (either high or low): <1.0 x 10³/mm³ (12), 1.0-19.9 x 10³/mm³: (0), ≥20 x 10³/mm³ (3)
-
AIDS - if the patient is HIV positive and suffers from complications, e.g., pneumocystis carinii pneumonia, Kaposi's sarcoma, lymphoma, tuberculosis, or toxoplasma infection (17)
-
Hematologic malignancy - e.g., lymphoma, acute leukemia, or multiple myeloma (10)
-
Metastatic cancer - if the metastasis is proven by, e.g., surgery, CT scan, MRI, or any other procedure (9)
If the patient has more than one condition (AIDS, hematologic malignancy, or metastatic cancer), choose the one with the most points assigned - the points don't add up.
-
Type of admission (in other words: reasons for hospitalization):
- Scheduled surgical - if the surgery was scheduled 24 hours or more prior to admission (0)
- Medical - if the patient hasn't undergone any surgical interventions within 1 week of admission (6)
- Unscheduled surgical - if the surgery was scheduled less than 24 hours prior to admission(8)
-
SAPS II calculator - a practical example
Let's show you how the calculator works! Imagine Rob, a 65 year old man, is referred to the ICU due to some complications and deterioration after being at the Internal Medicine Ward. He suffers from inoperable colon cancer with lung metastases and requires mechanical ventilation. His urine output in the last 8 hours was 400 ml, so, after calculations, it would be 400 ml * 3 = 1200 ml over 24 hours.
Therefore he receives:
- Age: 65 years old (12 points)
- Urine: 1200 ml (0 points)
- Metastatic cancer (9 points)
- Medical admission (6 points)
Here are his other parameters:
- Heart rate: 140 bpm (4 points)
- Systolic blood pressure: 105 mmHg (0 points)
- Temperature: 37.5oC (0 points)
- Glasgow Coma Score: 8 (13 points)
- PF ratio: 180 mmHg/% (9 points)
- BUN: 28 mg/dL (0 points)
- Na+: 135 mEq/L (0 points)
- K+: 4.0 mEq/L (0 points)
- Bicarbonate: 18 mEq/L (3 points)
- Bilirubin: 3.5 mg/dL (0 points)
- WBC: 18.3 x 103 (0 points)
After summing up all of the given points, his SAPS II score is 56 (out of 163 points).
Now we can calculate his ICU mortality rate:
X = −7.7631 + 0.0737 ∗ SAPS II points + 0.9971 ∗ ln(SAPS II points + 1)
Mortality = exp(X)/(1 + exp(X))
Where:
- ln(x) is a natural logarithm of x
His in-hospital mortality risk = 59.8 %
How to interpret the SAPS results for mortality risk assessment?
There's a sigmoidal relationship between mortality risk and the SAPS II points, as you can see in the graph below:
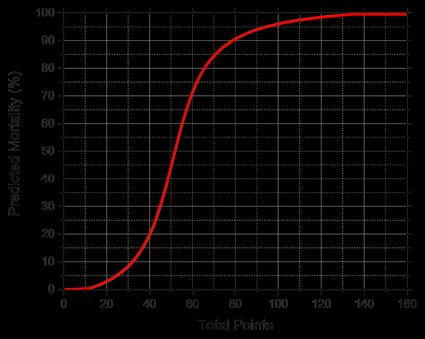
In the table you can compare how the risk of mortality changes with the numerical values of the SAPS II score:
Mortality | SAPS II points |
|---|---|
10% | 25 pts |
25% | 40 pts |
50% | 52 pts |
75% | 64 pts |
90% | 77 pts |
Who is SAPS II Calculator for?
This tool is for patients over the age of 15, admitted to Intensive Care Units. For each factor, you should use the value that scores the most points from the past 24 hours. The score can be calculated once per stay. However, if the patient is discharged from ICU and then readmitted, you can calculate a new SAPS II score.
The was conducted in 1991, with data collected from 12,997 patients from twelve different countries. Patients with burn injuries and cardiac problems were excluded from the study, which is why you shouldn't use this SAPS II calculator on patients with similar conditions.
Alternative ICU mortality rate calculations
-
If you need help with ICU mortality risk assessment, the is one solution. However, the APACHE II calculator is only applicable to patients newly admitted to the ICU (not ones transferred from a different department) or patients with liver failure or HIV.
-
With our qSOFA score calculator you can easily assess the mortality risk of a patient outside the ICU. It is intended to be used on patients with a life-threatening organ dysfunction due to an infection (sepsis).
-
In case the patient suffers from a community-acquired pneumonia (CAP), the CURB-65 calculator might become handy. It calculates the risk of death and helps decide whether the patient should be admitted to the hospital or not.
-
If a patient has a range of conditions and chronic diseases, the can be used. It contains nineteen categories of comorbidities and predicts the patient's ten-year mortality - it is applicable in any patient suffering from multiple diseases.
Be aware that the SAPS II mortality risk formula is not uniform for all ICUs and you should adapt it according to both patient-specific and centre-specific characteristics. It is not intended to determine an individual patient's chance of survival.